Categories
The Evolving Landscape of US Healthcare
Presented by Olson Research Group
In the past 6-9 months, the speed at which the US healthcare landscape is changing has accelerated. This cannot fully be attributed to the impact of Obamacare; rather it is more around what might be considered a seismic shift system wide. This impact can be seen and felt across the four largest stakeholders in the US Healthcare system-payers, physicians or providers, patients and manufacturers. Here we highlight some of these shifts which we feel will have the greatest impact on the marketing research industry as we brace to adjust with these trends.
The Payers
During 2012-2013 there was significant consolidation of healthcare plans and more pronounced growth in what were formerly called Integrated Delivery Networks (IDNs), now referred to as Accountable Care Organizations (ACOs). These IDNs or ACOs are the integration of multiple locations of healthcare into one centralized entity. With hospitals serving as the center or hub of care, satellite locations such as physician offices, outpatient
clinics, ambulatory centers, long term care facilities, radiology centers and infusion centers are the spokes emanating from that central location. This delivery model organizes all the 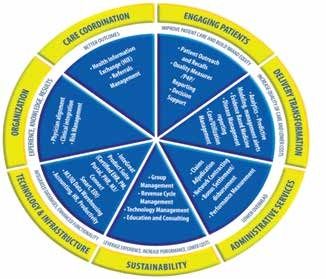
Previously disparate participants into one common unit. This, combined with the many state healthcare exchanges, is emerging as the delivery model of the future in the US. While the slow adoption of Obamacare has provided much media debate, there is no doubt that the means in which healthcare is delivered in the US is moving in a direction that much more closely aligns with the rest of the world – government guidance at the high level and a more
standardized model of delivery at the local level. At last count there were over 450 of these new ACO entities across the country – between those associated with CMS (Medicare Pioneers) and private shared savings groups. While some uncertainty remains as to how ACO’s will actually function, the model shown here by McKesson Healthcare illustrates their intended functionality.
Physicians
In the world of end healthcare providers, things are changing just as dramatically. Industry estimates contend that greater than 50% of Health Care Providers (HCPs) are now employees of some larger healthcare entity such as an ACO, with the expectation that this will grow to 70-80% over the next two to three years. The more progressive ACOs in the country are establishing very clear disease protocols for HCPs to follow. The resulting guidelines are an attempt to streamline medication choices (with a clear emphasis on generics) and ultimately simplify the treatment of chronically ill patients and to significantly restrict the use of high cost drugs. Many of these plans are also implementing systems of “report cards” whereby providers are scored on how they treat patients and even how patients score them on follow up and effective delivery of care. Recently Olson Research Group surveyed more than 1,200 healthcare professionals from their database. Providers gave feedback as to how the impending healthcare reforms were impacting their practices and what they felt about the future. The word cloud here captures the essence of their feedback.
 The complexion of the medical practices is just as fluid; large multi-specialty groups are becoming the standard, with Nurse Practitioners (NPs) and
The complexion of the medical practices is just as fluid; large multi-specialty groups are becoming the standard, with Nurse Practitioners (NPs) and
Physician Assistants (PAs) being utilized almost exclusively in first level triage of primary care patients. The adoption of electronic healthcare record (EHR) platforms is almost universal.
Those who have not adopted by the end of 2014 will not be paid for Medicaid and Medicare patients – currently over 50% of the US patient population and growing dramatically based
on demographics and economics. These EHR systems have the potential (although not fully realized yet) of collecting and communicating entire patient profiles and histories to massive
“big data” repositories for analysis and trending. Patients The patient was once just a passive recipient of healthcare – limited options, a simple prescription plan and more often
directed to a traditional hospital setting if an inpatient procedure was necessary. This too has evolved rapidly. With the emergence of mobile technology and all the healthcare apps that seem to spring up even daily, patients, or consumers of healthcare more aptly referred to, are barraged with more options for maintaining a healthy lifestyle than anyone could possibly avail themselves of. And while more patients are becoming active consumers of healthcare there are still significant gaps in terms of access and care consistency – hence the push for a patient protection affordable care act. A recent report cited that even in our well developed system of medical care, 20% of Americans still do not live in an area where there is adequate primary care coverage.
At this point in time it’s still far too early to predict any success or deficiencies in the plan being enacted, but an underlying wave of uncertainty abounds. As the photo 
here suggests – “We know something’s coming…we just don’t know what….”
Manufacturers
Biopharmaceutical manufacturers have experienced equally disruptive events and trends. Today pipelines are full of new and unique specialty drugs, many of which will be more effectively directed to the patients most receptive to them through companion diagnostics – the closest thing to real personalized medicines. The large Pharma companies are actively shedding assets that have historically consumed resources and potentially negatively affected operating income. Emerging from this are disease focused firms who are publicly acclaiming their intent to build portfolios in fewer therapeutic areas, but with deeper intellectual property. Alliances abound which will capitalize on smaller firms doing the early discovery and that big Multi-National Firms engaged more in late stage development,
manufacturing and ultimate distribution. Traditional sales forces will continue to shrink as the appetite for promotional activity wanes and formularies increasingly drive medication choices. In the end some of the draconian changes will lead the industry to a more productive and efficient outcome.
So What Does This All Mean?
As marketing research professionals, we must be able to understand the evolving industry trends so that we can remain valued suppliers to our clients. While there are no clear answers as to how we should navigate this new uncharted territory, we feel there are a series of guidelines that can help provide a framework in the new era:
• Every research engagement, whether for a product in development, one that’s peri-launch, or one that is focused on end of product life cycle, needs to contain a cohort of payers. More appropriately, it should consist of those who are formulary decision makers within an existing or emerging ACO.
• For qualitative work, moderators must be conversant in the nuances of payers’ structured environment to be able to tease out the finer details around product positioning and ultimate budgetary implications. A simple answer of, “it’s all about price” just cannot suffice for relevant and actionable feedback.
• When conducting research with the end providers of healthcare, the respondent population should consist of both MD degreed and non-degreed individuals. The future of healthcare delivery in the US is multidisciplinary and as such NPs, PAs, managers of practices, and other ancillary delivery professionals must be considered.
• Leveraging electronic healthcare report data will be the next major breakthrough in our industry. Some firms are beginning to understand how to harness that and they will be the purveyor of the “Big Data” solutions.
• Don’t omit the patient. The concept of analyzing the proverbial patient journey has become a common strategy.
But in today’s shifting environment, this takes on multiple levels and requires the ability to not only reach the right patients, but it mean may require aligning with advocacy groups in some of the rare and orphan disease categories.
As the US healthcare system evolves, the degree and manner in which pharmaceutical marketing research suppliers adapt is critical to their survival. Those who understand the implications of the changing landscape on providing answers to key business questions will deliver relevant, actionable results and, in turn, will adopt a 3600 view of the environment, thus bringing the greatest value to their end clients.
Presented by
LOCATION
Yardley, Pennsylvania
Featured Expert
Why choose Olson Research Group
Access to healthcare
Experienced PMs
In-house programming
Recruiting expertise
Precise targeting
Sign Up for
Updates
Get content that matters, written by top insights industry experts, delivered right to your inbox.